If I Had Placenta Previa Will I Get It Again
- Research article
- Open up Admission
- Published:
Gamble of placenta previa in 2d nascency later first birth cesarean section: a population-based study and meta-analysis
BMC Pregnancy and Childbirth book 11, Article number:95 (2011) Cite this commodity
Abstract
Background
Objective: To compare the run a risk of placenta previa at second nascency among women who had a cesarean section (CS) at first nascence with women who delivered vaginally.
Methods
Retrospective cohort written report of 399,674 women who gave birth to a singleton first and second baby between Apr 2000 and February 2009 in England. Multiple logistic regression was used to adapt the estimates for maternal historic period, ethnicity, deprivation, placenta previa at first birth, inter-birth interval and pregnancy complications. In addition, we conducted a meta-analysis of the reported results in peer-reviewed manufactures since 1980.
Results
The rate of placenta previa at 2nd birth for women with vaginal first births was four.4 per 1000 births, compared to 8.7 per 1000 births for women with CS at first birth. After adjustment, CS at start nascence remained associated with an increased risk of placenta previa (odds ratio = 1.lx; 95% CI ane.44 to 1.76). In the meta-analysis of 37 previously published studies from 21 countries, the overall pooled random furnishings odds ratio was ii.20 (95% CI 1.96-2.46). Our results from the current written report is consistent with those of the meta-analysis as the pooled odds ratio for the half-dozen population-based cohort studies that analyzed 2d births only was i.51 (95% CI ane.39-one.65).
Conclusions
At that place is an increased risk of placenta previa in the subsequent pregnancy afterward CS delivery at get-go birth, simply the risk is lower than previously estimated. Given the placenta previa charge per unit in England and the adjusted effect of previous CS, 359 deliveries by CS at kickoff birth would result in one additional example of placenta previa in the next pregnancy.
Background
Placenta previa can have serious agin consequences for both mother and baby, including an increased take chances of maternal and neonatal mortality[i–iii], fetal growth restriction and preterm commitment[4], antenatal and intrapartum hemorrhage[5–7], and women may require a blood transfusion[8] or even an emergency hysterectomy. It is a relatively uncommon condition, with an overall incidence in England of half-dozen.iii per grand births[9], but incidence rates are higher amid women with advanced maternal age, multiple gestation, loftier parity, or who smoke or use illegal drugs[10]. The take a chance of placenta previa is likewise reported to be college among women with previous uterine surgery, including cesarean section[xi].
In England, cesarean sections constituted 25% of National Health Service (NHS) deliveries during 2010, and the rates have been rising for both main and emergency CS[9]. The run a risk of placenta previa in a pregnancy after a CS delivery has been reported to be between 1.five and 6 times higher than later on a vaginal delivery. A meta-analysis of studies published before 2000 of previous CS every bit a hazard factor for placenta previa found an overall odds ratio of 2.7 [10]. However, the overall odds ratio was lower in studies that had better adjustment for confounders[ten]. A recent study from the USA that was not included in the meta-analysis, and which used a population-based cohort of 11 meg pregnancies, found an adjusted odds ratio of 1.8 for all pregnancies[12] and an adapted odds ratio of ane.5 for 2d births only[13].
Testify well-nigh the risk of placenta previa following a previous CS in Great britain women is express to results published 25 years ago[fourteen]. We used the Hospital Episode Statistics (HES), an authoritative database of all admissions to NHS hospitals in England, to define a population-based cohort and to quantify the association betwixt CS at starting time birth and the adventure of developing placenta previa in the subsequent pregnancy. We likewise performed a meta-analysis of the reported results in peer-reviewed articles since 1980.
Methods
The cohort report
We used the HES dataset for 9 financial years from April 2000 to February 2009 for the cohort study. In HES, individual patients are allocated the same identifier for each episode of care[nine] and core fields contain patient demographics, clinical information, and hospital administrative information. Diagnostic information is coded using the International Nomenclature of Diseases 10th revision (ICD10) and operative procedures are coded using the UK Office for Population Censuses and Surveys classification, fourth revision (OPCS4). For delivery episodes, the HES dataset also has an additional "motherhood tail" which includes parity, birth weight, gestational age, method of commitment, and pregnancy event. Yet, not all records that describe a delivery episode have data entered into this tail.
All women who gave birth to a singleton starting time and second baby from 1st April 2000 to 28thursday February 2009 were eligible for inclusion. A delivery was defined as an episode of intendance that included a relevant OPCS4 lawmaking (R17-R25) or ICD10 code (O80-O84) for the style of delivery, or a maternity tail with a valid engagement of nativity for a babe. Deliveries were coded as a cesarean section by the relevant OPCS4 codes (R17 for primary CS or R18 for emergency CS) or if OPCS4 codes were not available, by the commitment method specified in the maternity tail. If neither of the sets of codes were available (0.5% of commitment episodes), vaginal delivery was causeless.
We confined the analysis to NHS trusts (astute hospital organizations) that had a reasonable level of data completeness on parity, defined as having parity information in the maternity tail for more than than 50% of the delivery episodes in at least seven of the ix years covered in the written report. NHS trusts were included if the proportion of nulliparous women in that trust was between 25% and 55% (which corresponded to the overall rate in England and Wales ± 15%[xv]) to remove hospitals with poor data quality. Women were allocated to the NHS trusts that existed in February 2009 to take business relationship of previous organizational mergers.
We used the HES patient identifier to trace the 2nd births of those women who had been recorded as nulliparous and who had singleton first births in identified NHS trusts. Diagnostic information for the second birth was taken from the core HES diagnosis fields. Cases of placenta previa were identified by the ICD10 lawmaking O44. Pregnancy complications were identified using ICD10 codes O10, O11, O16 for pre-existing hypertension; O13 for gestational hypertension; O14 and O15 for pre-eclampsia and eclampsia; O24.iv and O24.nine for gestational diabetes; and O40 for polyhydramnios.
The event of previous CS delivery on the chance of placenta previa was estimated using unadjusted and adapted odds ratios. Multiple logistic regression was used to calculate the odds ratios and the take a chance of placenta previa adjusted for maternal age (<twenty, 20-29, xxx-39, ≥40), maternal ethnicity (White, Asian, Black and Other), deprivation, inter-nascence interval (<1, i-two, 2-3, 3-4, iv-5, ≥five years), placenta previa at get-go nascency and indicators for pregnancy complications (i.eastward., pre-existing hypertension, gestational hypertension including pre-eclampsia and eclampsia, gestational diabetes and polyhydramnios). Deprivation was measured using the 2004 Index of Multiple Deprivation (IMD) rank of the English Super Output Areas. The IMD combines a range of economical, social and housing indicators into a single deprivation score for each small expanse in England [xvi]. Categories were defined by partition the ranks of the 32,480 areas into quintiles (0-20th percentiles, 20-40th percentiles, etc.) and labeled i (least deprived) to 5 (nearly deprived). Women were allocated a category based on their region of residence. We calculated the number needed to impairment using the adjusted estimates from the logistic regression[17].
Nosotros examined whether the effect of CS on placenta previa rates was related to the level of other gamble factors, such equally whether the effect of CS on the placenta previa take chances differed between younger and older women. The significance of an interaction term between previous CS and other risk factors was assessed with the likelihood ratio test. All analyses were done in Stata/SE x.0.
The study is exempt from IRB and Britain NREC approval every bit information technology involved analysis of an existing dataset comprising data on delivery episodes for women who cannot be identified directly or through the HES patient numbers linked to them.
Review of literature and meta-assay
We searched Pubmed, Embase, Web of Science, Cinahl and the Cochrane Library for the period January 1980 to Jan 2011 to identify studies that examined the relationship betwixt previous cesarean section and placenta previa. The keywords of "placenta previa"/"placenta praevia" and "cesarean"/"caesarean" were searched in MESH headings, titles and abstracts to locate relevant manufactures. We also checked the references of the selected articles and previous reviews. Nosotros only included articles written in English language and limited the search to peer-reviewed journals.
We selected studies in which placenta previa was diagnosed or recorded at third trimester or during commitment. If two or more relevant articles used the same data source in overlapping years, nosotros selected the study that adjusted the result size by age or parity, and if there is even so replication, the study with the larger sample size.
Estimated log odds ratios and standard errors of log odds ratios were calculated from raw information presented in the included papers. The meta-analysis was performed using a random-effects model, and summarized the degree of consistency beyond the study results using the I2 measure, the percentage of total variation across studies that is due to heterogeneity rather than hazard[xviii]. Meta-regression was used to assess whether the event size was associated with engagement of publication, written report design (cohort vs. case-command), source of data (population vs. hospital based), method of diagnosis of placenta previa (confirmed at delivery vs. recorded at hospital or birth registry databases), and whether the results were adjusted for age and parity. We also did a subgroup analysis of population-based cohort studies focusing on the clan between first-birth cesarean delivery and 2nd-birth placenta previa and compared the magnitude of this association with the results from our cohort.
Results
The cohort study
Between April 2000 and Feb 2009, there were 4,987,245 singleton delivery episodes in 146 English NHS trusts. It was necessary to exclude 76 NHS trusts due to incomplete parity information. This left 2,484,468 (49.8%) singleton delivery episodes in 70 NHS trusts. Of these, 958,882 (38.6%) women were nulliparous and 399,674 had had a 2d singleton nativity by February 2009. The overall charge per unit of placenta previa for the accomplice at first nativity was three.half-dozen and at second birth was 5.3 per 1000 births. The proportion of women who had undergone a CS at first birth was 21.5%. The median birthweight at second nascence was 3448 grams (Interquartile range: 3110 -3780 grams).
The charge per unit of placenta previa at second birth was iv.4 per thousand births for women with vaginal delivery at outset birth and eight.vii for women with CS at first birth (unadjusted odds ratio = 1.88). We found that this increased risk of placenta previa persisted after other hazard factors were taken into account (adjusted odds ratio = i.threescore) (Table 1). The strongest clan between a maternal characteristic and the chance of placenta previa was for women who had placenta previa at first birth (adjusted odds ratio = four.77). Women with advanced maternal age, with polyhydramnios, with very short nascence intervals of less than one year, and with birth intervals of more than four years also had college placenta previa risks. Women with pre-existing hypertension had lower placenta previa risks. Using these estimates, nosotros expect that 359 CS deliveries at first nascency would consequence in one additional case of placenta previa at second nativity.
Individual interactions with categories for maternal historic period, ethnicity, deprivation, maternal risk factors and inter-pregnancy interval did non alter the size of the effect of a previous CS on the take a chance of placenta previa.
Review of literature and meta-analysis
We identified 2077 manufactures of which 74 were of potential relevance to merit a full-text review. 41 articles were selected for inclusion in the review, and an boosted 8 manufactures were retrieved from reference lists [8, 12, 13, 19–64]. Among the 49 articles, 12 used overlapping datasets with other studies and were excluded. Study characteristics are presented in Table 2 and the meta-analysis results from the selected 37 studies are given in Effigy ane. The overall pooled random effects odds ratio was ii.20 (95% CI 1.96-2.46). The spread of the odds ratios reported in the private studies were larger than tin can be expected past run a risk alone (Itwo= 87.6%).
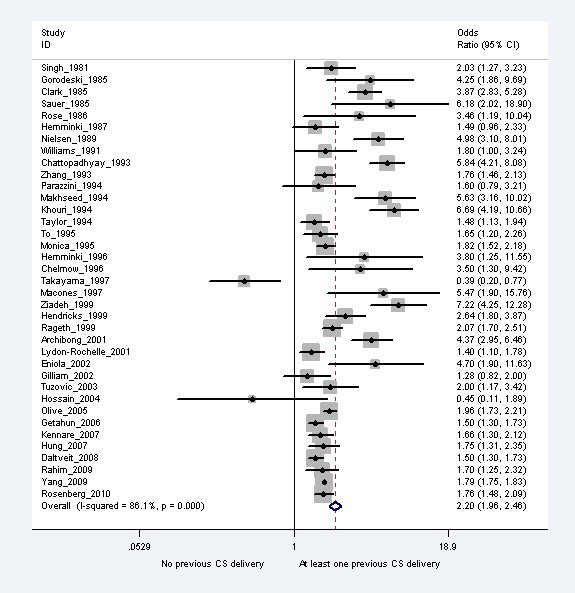
The relative risk of placenta previa associated with a previous cesarean section.
In bi-variate meta-regressions of various study characteristics on the reported odds ratios (Table 3), significantly smaller effect size of previous cesarean department on placenta previa was associated with contempo studies (p = 0.04), population-based studies (p = 0.03), and those that adjusted for historic period and parity (p = 0.04). The odds ratios reported in the individual studies were not associated with type of written report design (accomplice vs. instance-command) and method of diagnosis of placenta previa (data tape in database vs. confirmation at delivery). Heterogeneity beyond studies remained in subgroup analyses by study design, setting and timing of diagnosis of placenta previa. Results from studies that adjusted for age and parity were less heterogeneous (Itwo = 52.3%) and the variation in the results from studies that analyzed first 2 births were due to take chances lonely (Iii = 0%).
The pooled random effects odds ratio for the half dozen population-based accomplice studies analyzing second births only was 1.51 (95% CI ane.39-1.65, Iii = 0%), comparable to our cohort study.
The pooled odds ratio and association of report characteristics on the odds ratio remained similar after inclusion of the current study in the meta-analysis. The subgroup of studies analyzing first 2 births had significantly smaller effect sizes (p = 0.04).
Discussion and Conclusions
Among women in England, cesarean department in the first commitment increased the take chances of placenta previa in the subsequent delivery past 60%. There was no evidence that the event of CS on placenta previa rates varied among different groups of women or by the time between two pregnancies. The risks of placenta previa in the 2nd pregnancy also increased by previous placenta previa, advanced maternal historic period and with birth intervals of less than 1 year or more four years. Women with pre-existing hypertension were less probable to have placenta previa. Our results are consistent with recent studies from other countries which typically plant odds ratios ranging from 1.4 to ane.7.
Strengths and limitations of this study
This is the offset written report of placenta previa risk in England using a large, population-based cohort of nearly 400,000 women with first two births. It included half of all singleton NHS hospital deliveries betwixt April 2000 and February 2009. Due to its comprehensive coverage, the HES database is a valuable resources specially for studies of relatively uncommon conditions such as placenta previa.
In this study we focused only on the effect of a CS delivery at first birth on a second pregnancy. This has two benefits. First, it corresponds to the information typically required past women and obstetricians. For instance, the average achieved family size in the UK is approximately two[65], and so the effect of CS on the 2d birth is more relevant and authentic than a relative hazard based on all pregnancies that may include women with multiple previous CS. Second, estimates based on all pregnancies volition be influenced by the proportions of women in iind, 3rd, fourthursday... pregnancies contained in the study sample. Written report samples may too differ in the observed sequences of modes of commitment (for example, due to differences in the propensity of local women to opt for trial of labor). Both factors volition reduce the comparability of the estimates across studies. Nosotros note that, while in that location is a wide range of reported relative risks, at that place is consistency in the effect sizes for studies express to second births.
It is possible that the women with incomplete data in the maternity tail differed from women included in the study in terms of their characteristics and pregnancy risks. However, the distributions of maternal age and mode of delivery were similar in the episodes with good quality data and omitted episodes, which suggests the risk of selection bias is likely to exist small.
The coding of the diagnoses and procedures in administrative databases is potentially inaccurate. However, this is unlikely to have had a major effect in our study because previous studies accept reported high-levels of agreement in the coding of cesarean department between administrative databases and medical reviews (kappa > 0.98, where stated) [66–68]. Furthermore, cesarean deliveries were divers using the offset 3 characters of the full 4-character OPCS codes, and broader categories rather than specific codes have been shown to exist more reliable[69].
But like other population-based studies, we were non able to confirm the grade and severity of placenta previa [seventy, 71]. We were also not able to control for behavioral hazard factors, such as maternal smoking and alcohol and drug utilize, and previous abortions [40, 72–74]. Nonetheless, the effects of these take a chance factors equally reported in the literature are minor compared to the effect of prior CS, maternal age and parity[10].
Comparison with other studies
In the previous meta-analysis of 21 studies, the pooled odds ratios of previous CS as a risk gene for placenta previa was found to exist 2.7 (95% CI: ii.3 to 3.ii). The same study emphasized that the odds ratios were highly variable by setting, study blueprint, sample size and quality. For well-designed studies, the pooled odds ratio was ane.ix (95% CI: 1.vii to 2.2)[10].
Since this review, a number of studies have been published. 13 of the 37 studies included in our meta-analysis are mail service-2000 and comprehend approximately 12 million women. The pooled odds-ratio of 2.2 (95% CI: 2.0 to 2.5) from this meta-assay is less than the previous review, and reflects the fact that studies with contempo publication dates institute smaller issue sizes.
Our results for the English language cohort are in agreement with other recent, population-based cohorts analyzing 2nd-births only. In the largest population-based cohort study of over xi million singleton deliveries between 1995 and 2000 in the USA, the adjusted odds ratio of the outcome of previous CS on placenta previa at second-nativity was one.five[75]. Other population-based cohort studies published in the last decade reported adjusted odds ratios ranging from 1.4 to one.vii, using Missouri state birth certificates data[26], Washington land Birth Events data[viii], South Australian Perinatal Data[37] and Medical Birth Registry of Norway[49]. A population-based study using information from the Swedish Birth Registry institute a higher adjusted odds ratio of 1.8, but this study did not adequately command for risk factors[76].
A few studies have investigated whether the result of a previous CS on the hazard of placenta previa was modified by other risk factors. The Missouri cohort written report found that the consequence of CS was 70% higher for women with a 2nd pregnancy within a year after the start delivery[26]. We did not discover evidence to support the hypothesis that inter-pregnancy interval influences the size of effect of offset birth CS. Our results are consistent with the Washington country cohort study that found the size of event of CS was not influenced by maternal age at 2nd birth [8].
Implications for policy and practice
Cesarean section rates are rising worldwide, and an increase in the longer term complications of CS should be anticipated. The presumed short and long term safety of CS is probably one of the factors underlying both the growing rate of CS and the wide variation in CS rates not deemed for past instance mix. There is a demand for better understanding of the relative risks associated with vaginal and CS births to back up determination-making by mothers and clinicians[77].
The Confidential Enquiry into Maternal and Child Wellness recommends that women with a prior CS should have placental localization in current pregnancy to exclude placenta previa[78]. If placenta previa is diagnosed, there must be farther investigation to exclude placenta accreta, a potentially life-threatening status. In high-income countries, advanced radiological facilities can help to diagnose this serious condition in antenatal care and to plan delivery in a tertiary care unit of measurement. However, in depression or middle-income countries, placental conditions may exist encountered first time at the CS with its serious consequences and it is imperative that senior and experienced doctors are involved in the care of women with placenta previa from the outset.
Our study has demonstrated that, in improver to women with previous CS, women with advanced maternal age, women with birth intervals of less than one yr and women who had a previous placenta previa are at a college risk of developing placenta previa. Nonetheless, our written report suggests that the accented take chances remains pocket-size. Women who had placenta previa in their previous pregnancy were at the greatest take chances of placenta previa in a electric current pregnancy but less than v in 100 of women with a previous placenta previa would exist expected to have this complication again. Clinicians should consider and communicate these factors when counseling their patients using appropriate and simplified risk statistics[79]. Our study quantifies this risk and provides data that tin exist used to reassure women, attending for pre-conception counseling clinics or antenatal clinics as well as in pre-operative consent discussions for women undergoing CS.
References
-
Salihu HM, Li Q, Rouse DJ, Alexander GR: Placenta previa: Neonatal expiry after live births in the United States. Am J Obstet Gynecol. 2003, 188 (5): 1305-1309. 10.1067/mob.2003.303.
-
Ananth CV, Smulian JC, Vintzileos AM: The event of placenta previa on neonatal bloodshed: a population-based study in the United states of america, 1989 through 1997. Am J Obstet Gynecol. 2003, 188 (five): 1299-1304. ten.1067/mob.2003.76.
-
Iyasu S, Saftlas AK, Rowley DL, Koonin LM, Lawson HW, Atrash HK: The Epidemiology of Placenta-Previa in the United-States, 1979 Through 1987. Am J Obstet Gynecol. 1993, 168 (5): 1424-1429.
-
Ananth CV, Demissie Yard, Smulian JC, Vintzileos AM: Relationship among placenta previa, fetal growth restriction, and preterm delivery: A population based study. Obstet Gynecol. 2001, 98 (two): 299-306. x.1016/S0029-7844(01)01413-ii.
-
Brace V, Kernaghan D, Penney K: Learning from adverse clinical outcomes: major obstetric haemorrhage in Scotland, 2003-05. BJOG. 2007, 114 (eleven): 1388-1396. 10.1111/j.1471-0528.2007.01533.x.
-
Crane JMG, Van den Hof MC, Dodds L, Armson BA, Liston R: Maternal complications with placenta previa. Am J Perinatol. 2000, 17 (2): 101-105. 10.1055/due south-2000-9269.
-
Bhide A, Prefumo F, Moore J, Hollis B, Thilaganathan B: Placental edge to internal os altitude in the late third trimester and way of delivery in placenta praevia. BJOG. 2003, 110 (9): 860-864. 10.1111/j.1471-0528.2003.02491.x.
-
Lydon-Rochelle M, Holt VL, Easterling TR, Martin DP: First-birth cesarean and placental abruption or previa at second nativity. Obstet Gynecol. 2001, 97 (five): 765-769. 10.1016/S0029-7844(01)01121-eight.
-
HESOnline. 2011, [http://www.hesonline.nhs.u.k./]
-
Faiz Every bit, Ananth CV: Etiology and risk factors for placenta previa: an overview and meta-analysis of observational studies. J Matern Fetal Neonatal Med. 2003, 13 (three): 175-190. 10.1080/jmf.13.3.175.190.
-
Ananth CV, Smulian JC, Vintzileos AM: The clan of placenta previa with history of cesarean delivery and abortion: A metaanalysis. Am J Obstet Gynecol. 1997, 177 (v): 1071-1078. 10.1016/S0002-9378(97)70017-6.
-
Yang Q, Wen SW, Phillips Thousand, Oppenheimer L, Black D, Walker MC: Comparing of maternal risk factors between placental abruption and placenta previa. American Periodical of Perinatology. 2009, 26 (4): 279-286. x.1055/s-0028-1103156.
-
Yang Q, Wen SW, Oppenheimer L, Chen XK, Black D, Gao J, Walker MC: Association of caesarean delivery for kickoff birth with placenta praevia and placental abruption in second pregnancy. BJOG: An International Journal of Obstetrics and Gynaecology. 2007, 114 (5): 609-613. x.1111/j.1471-0528.2007.01295.x.
-
Rose GL, Chapman MG: Aetiological factors in placenta praevia--a instance controlled study. Br J Obstet Gynaecol. 1986, 93 (6): 586-588.
-
ONS: Birth statistics: Births and patterns of family unit building England and Wales (FM1) FM1 No. 36. Table 1.9 Components of total fertility rates1: occurrence inside/exterior England and Wales matrimony, birth order and age of mother, 1997-2007. 2007
-
Office of the Deputy Prime Minister. The English indices of deprivation 2004: summary (revised). [http://www.communities.gov.britain/documents/communities/pdf/131206.pdf]
-
Bough R, Kuss O, Hildebrandt G, Gehrmann U: Estimating adapted NNT measures in logistic regression analysis. Stat Med. 2007, 26 (30): 5586-5595. x.1002/sim.3061.
-
Higgins JP, Thompson SG: Quantifying heterogeneity in a meta-analysis. Stat Med. 2002, 21 (11): 1539-1558. 10.1002/sim.1186.
-
Abu-Heija AT, El-Jallad F, Ziadeh South: Placenta previa: Effect of historic period, gravidity, parity and previous caesarean section. Gynecologic and Obstetric Investigation. 1999, 47 (i): 6-8. 10.1159/000010053.
-
Archibong EI, Ahmed ESM: Risk factors, maternal and neonatal outcome in major placenta previa: A prospective study. Annals of Saudi Medicine. 2001, 21 (iii-four): 245-247.
-
Chattopadhyay SK, Kharif H, Sherbeeni MM: Placenta praevia and accreta after previous caesarean section. European Journal of Obstetrics Gynecology and Reproductive Biology. 1993, 52 (3): 151-156. 10.1016/0028-2243(93)90064-J.
-
Chelmow D, Andrew DE, Baker ER: Maternal cigarette smoking and placenta previa. Obstetrics and Gynecology. 1996, 87 (five I): 703-706.
-
Clark SL, Koonings PP, Phelan JP: Placenta previa/accreta and prior cesarean section. Obstetrics and Gynecology. 1985, 66 (1): 89-92.
-
Daltveit AK, Tollanes MC, Pihlstrom R, Irgens LM: Cesarean delivery and subsequent pregnancies. Obstetrics and Gynecology. 2008, 111 (6): 1327-1334. x.1097/AOG.0b013e3181744110.
-
Eniola AO, Bako AU, Selo-Ojeme Exercise: Risk factors for placenta praevia in southern Nigeria. E Afr Med J. 2002, 79 (10): 535-538.
-
Getahun D, Oyelese Y, Salihu HM, Ananth CV: Previous cesarean delivery and risks of placenta previa and placental abruption. Obstet Gynecol. 2006, 107 (iv): 771-778. 10.1097/01.AOG.0000206182.63788.fourscore.
-
Gilliam 1000, Rosenberg D, Davis F: The likelihood of placenta previa with greater number of cesarean deliveries and higher parity. Obstetrics and Gynecology. 2002, 99 (half-dozen): 976-980. x.1016/S0029-7844(02)02002-1.
-
Gorodeski IG, Bahari CM: The issue of placenta previa localization upon maternal and fetal-neonatal outcome. J Perinat Med. 1987, fifteen (two): 169-177. ten.1515/jpme.1987.fifteen.2.169.
-
Gorodeski IG, Neri A, Bahary CM: Placenta previa - The identification of depression- and high-chance subgroups. European Periodical of Obstetrics Gynecology and Reproductive Biology. 1985, twenty (3): 133-143. 10.1016/0028-2243(85)90012-7.
-
Handler AS, Mason ED, Rosenberg DL, Davis FG: The relationship between exposure during pregnancy to cigarette smoking and cocaine apply and placenta previa. Am J Obstet Gynecol. 1994, 170 (three): 884-889.
-
Hemminki Eastward: Pregnancy and birth later cesarean section: a survey based on the Swedish birth annals. Nativity. 1987, 14 (ane): 12-17. 10.1111/j.1523-536X.1987.tb01443.x.
-
Hemminki E, Merilainen J: Long-term effects of cesarean sections: Ectopic pregnancies and placental issues. American Journal of Obstetrics and Gynecology. 1996, 174 (5): 1569-1574. ten.1016/S0002-9378(96)70608-7.
-
Hendricks MS, Grub YH, Bhagavath B, Singh K: Previous cesarean section and abortion as risk factors for developing placenta previa. Journal of Obstetrics and Gynaecology Inquiry. 1999, 25 (2): 137-142. 10.1111/j.1447-0756.1999.tb01136.x.
-
Hershkowitz R, Fraser D, Mazor M, Leiberman JR: One or multiple previous cesarean sections are associated with similar increased frequency of placenta previa. European Periodical of Obstetrics Gynecology and Reproductive Biological science. 1995, 62 (2): 185-188. 10.1016/0301-2115(95)02194-C.
-
Hossain GA, Islam SM, Mahmood S, Chakraborty RK, Akhter N, Sultana S: Placenta previa and information technology's relation with maternal age, gravidity and cesarean section. Mymensingh Med J. 2004, thirteen (two): 143-148.
-
Hung Thursday, Hsieh CC, Hsu JJ, Chiu TH, Lo LM, Hsieh TT: Risk factors for placenta previa in an Asian population. Int J Gynaecol Obstet. 2007, 97 (1): 26-30. 10.1016/j.ijgo.2006.12.006.
-
Kennare R, Tucker Yard, Heard A, Chan A: Risks of adverse outcomes in the next nascence after a first cesarean commitment. Obstetrics and Gynecology. 2007, 109 (two Part 1): 270-276.
-
Khouri JA, Sultan MG: Previous caesarean section and the ascent incidence of placenta praevia and placenta accreta. Journal of Obstetrics and Gynaecology. 1994, xiv (one): 14-sixteen. 10.3109/01443619409025956.
-
Kramer Md, Taylor V, Hickok DE, Daling JR, Vaughan TL, Hollenbach KA: Maternal smoking and placenta previa. Epidemiology. 1991, 2 (3): 221-223. 10.1097/00001648-199105000-00012.
-
Macones GA, Sehdev HM, Parry S, Morgan MA, Berlin JA: The association between maternal cocaine use and placenta previa. Am J Obstet Gynecol. 1997, 177 (5): 1097-1100. 10.1016/S0002-9378(97)70022-X.
-
Makhseed K, El-Tomi N, Moussa Grand: A retrospective assay of pathological placental implantation - Site and penetration. International Journal of Gynecology and Obstetrics. 1994, 47 (2): 127-134. 10.1016/0020-7292(94)90352-2.
-
McMahon MJ, Li R, Schenck AP, Olshan AF, Royce RA: Previous cesarean nascency: A risk factor for placenta previa?. Journal of Reproductive Medicine for the Obstetrician and Gynecologist. 1997, 42 (seven): 409-412.
-
Monica G, Lilja C: Placenta previa, maternal smoking and recurrence chance. Acta Obstet Gynecol Scand. 1995, 74 (5): 341-345. x.3109/00016349509024425.
-
Nielsen TF, Hagberg H, Ljungblad U: Placenta previa and antepartum hemorrhage after previous cesarean section. Gynecologic and Obstetric Investigation. 1989, 27 (2): 88-90. 10.1159/000293625.
-
Olive EC, Roberts CL, Algert CS, Morris JM: Placenta praevia: Maternal morbidity and identify of birth. Australian and New Zealand Journal of Obstetrics and Gynaecology. 2005, 45 (half dozen): 499-504. ten.1111/j.1479-828X.2005.00485.x.
-
Parazzini F, Dindelli M, Luchini L, La Rosa M, Potenza MT, Frigerio L, Ferrari A: Take chances factors for placenta praevia. Placenta. 1994, 15 (3): 321-326. 10.1016/0143-4004(94)90023-X.
-
Rageth JC, Juzi C, Grossenbacher H: Delivery afterwards previous cesarean: A take chances evaluation. Obstetrics and Gynecology. 1999, 93 (three): 332-337. 10.1016/S0029-7844(98)00446-3.
-
Rahim R, Shafqat T, Fayyaz South: An analysis of association of scarred uterus with placenta praevia and morbid adherence of placenta. Periodical of Medical Sciences. 2009, 17 (ii): threescore-63.
-
Rasmussen S, Albrechtsen S, Dalaker 1000: Obstetric history and the risk of placenta previa. Acta Obstetricia et Gynecologica Scandinavica. 2000, 79 (half dozen): 502-507. ten.1080/j.1600-0412.2000.079006502.ten.
-
Rose GL, Chapman MG: Aetiological factors in placenta praevia - a case controlled study. British Journal of Obstetrics and Gynaecology. 1986, 93 (half-dozen): 586-588.
-
Sauer Grand, Parsons M, Sampson G: Placenta previa: An analysis of three years experience. American Journal of Perinatology. 1985, 2 (one): 39-42. ten.1055/southward-2007-999909.
-
Sheiner E, Shoham-Vardi I, Hallak M, Hershkowitz R, Katz M, Mazor M: Placenta previa: Obstetric chance factors and pregnancy issue. Periodical of Maternal Fetal Medicine. 2001, x (vi): 414-419. 10.1080/jmf.ten.6.414.419.
-
Singh PM, Rodrigues C, Gupta AN: Placenta previa and previous cesarean department. Acta Obstetricia et Gynecologica Scandinavica. 1981, threescore (4): 367-368. 10.3109/00016348109154125.
-
Takayama T, Minakami H, Koike T, Watanabe T, Sato I: Risks associated with cesarean sections in women with placenta previa. Journal of Obstetrics and Gynaecology Research. 1997, 23 (four): 375-379.
-
Taylor VM, Kramer Medico, Vaughan TL, Peacock S: Placental previa in relation to induced and spontaneous abortion: a population-based written report. Obstet Gynecol. 1993, 82 (1): 88-91.
-
Taylor VM, Kramer MD, Vaughan TL, Peacock South: Placenta previa and prior cesarean delivery: How strong is the association?. Obstetrics and Gynecology. 1994, 84 (one): 55-57.
-
Taylor VM, Peacock Southward, Kramer Doc, Vaughan TL: Increased risk of placenta previa amid women of Asian origin. Obstetrics and Gynecology. 1995, 86 (5): 805-808. 10.1016/0029-7844(95)00262-P.
-
To WWK, Leung WC: Placenta previa and previous cesarean section. International Journal of Gynecology and Obstetrics. 1995, 51 (1): 25-31. 10.1016/0020-7292(95)80004-V.
-
Tuzovic Fifty, Djelmis J, Ilijic M: Obstetric Take a chance Factors Associated with Placenta Previa Evolution: Example-Control Study. Croatian Medical Journal. 2003, 44 (half-dozen): 728-733.
-
Williams MA, Mittendorf R, Lieberman Eastward, Monson RR, Schoenbaum SC, Genest DR: Cigarette smoking during pregnancy in relation to placenta previa. Am J Obstet Gynecol. 1991, 165 (1): 28-32.
-
Zhang J, Fried DB: Relationship of maternal smoking during pregnancy to placenta previa. American Periodical of Preventive Medicine. 1992, 8 (5): 278-282.
-
Zhang J, Savitz DA: Maternal age and placenta previa: A population-based, case-control study. American Periodical of Obstetrics and Gynecology. 1993, 168 (2): 641-645.
-
Ziadeh SM, Abu-Heija AT, El-Jallad MF: Placental praevia and accreta: An analysis of 2-years' feel. Journal of Obstetrics and Gynaecology. 1999, xix (6): 584-586. 10.1080/01443619963770.
-
Rosenberg T, Pariente Chiliad, Sergienko R, Wiznitzer A, Sheiner E: Critical analysis of take chances factors and outcome of placenta previa. Arch Gynecol Obstet. 2010
-
Jefferies J: Fertility assumptions for the 2006-based national population projections. Popul Trends. 2008, 131: 19-27.
-
Roberts CL, Bell JC, Ford JB, Morris JM: Monitoring the quality of maternity intendance: how well are labour and commitment events reported in population wellness data?. Paediatr Perinat Epidemiol. 2009, 23 (2): 144-152. 10.1111/j.1365-3016.2008.00980.10.
-
Lydon-Rochelle M, Holt VL, Easterling TR, Martin DP: Chance of uterine rupture during labor among women with a prior cesarean delivery. Due north Engl J Med. 2001, 345 (1): 3-viii. x.1056/NEJM200107053450101.
-
Yasmeen S, Romano PS, Schembri ME, Keyzer JM, Gilbert WM: Accuracy of obstetric diagnoses and procedures in hospital discharge information. Am J Obstet Gynecol. 2006, 194 (four): 992-1001. 10.1016/j.ajog.2005.08.058.
-
Dixon J, Sanderson C, Elliott P, Walls P, Jones J, Petticrew M: Assessment of the reproducibility of clinical coding in routinely collected hospital activity information: a study in two hospitals. J Public Wellness Med. 1998, 20 (1): 63-69.
-
Dola CP, Garite TJ, Dowling DD, Friend D, Ahdoot D, Asrat A: Placenta previa: Does its type affect pregnancy outcome?. Am J Perinatol. 2003, xx (vii): 353-360.
-
Tuzovic L: Complete versus incomplete placenta previa and obstetric outcome. Int J Gynecol Obstet. 2006, 93 (2): 110-117. ten.1016/j.ijgo.2006.02.006.
-
Ananth CV, Savitz DA, Luther ER: Maternal cigarette smoking as a chance gene for placental abruption, placenta previa, and uterine bleeding in pregnancy. Am J Epidemiol. 1996, 144 (9): 881-889.
-
Williams MA, Mittendorf R, Lieberman E, Monson RR, Schoenbaum SC, Genest DR: Cigarette-Smoking During Pregnancy in Relation to Placenta Previa. Am J Obstet Gynecol. 1991, 165 (one): 28-32.
-
Handler AS, Mason ED, Rosenberg DL, Davis FG: The Relationship Betwixt Exposure During Pregnancy to Cigarette-Smoking and Cocaine Employ and Placenta-Previa. Am J Obstet Gynecol. 1994, 170 (iii): 884-889.
-
Yang Q, Wen S, Oppenheimer L, Chen Ten, Black D, Gao J, Walker Thou: Clan of caesarean commitment for first nascence with placenta praevia and placental abruption in second pregnancy. BJOG. 2007, 114 (5): 609-613. x.1111/j.1471-0528.2007.01295.10.
-
Monica G, Lilja C: Placenta Previa, Maternal Smoking and Recurrence Risk. Acta Obstet Gynecol Scand. 1995, 74 (five): 341-345. 10.3109/00016349509024425.
-
Caesarean Sections. 2002, London: The Parliamentary Part of Science and Technology
-
Lewis G, (ed): The Confidential Research into Maternal and Child Health (CEMACH). Saving Mothers' Lives: reviewing maternal deaths to make motherhood safer - 2003-2005. The Seventh Study on Confidential Enquiries into Maternal Deaths in the United Kingdom. 2007, London: CEMACH
-
Spiegelhalter DJ: Understanding uncertainty. Ann Fam Med. 2008, 6 (3): 196-197. ten.1370/afm.848.
Pre-publication history
-
The pre-publication history for this paper can be accessed here:http://www.biomedcentral.com/1471-2393/11/95/prepub
Acknowledgements
We thank the Department of Health for providing the Hospital episode statistics data used in this report. IGU is supported past the Royal College of Obstetricians and Gynaecologists.
Author information
Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they take no competing interests.
Authors' contributions
All authors have fulfilled all weather required for authorship. IGU, GCS, LCE, DC, JvdM and TAM designed the study. IGU analyzed the data supported past DC and JvdM. IGU wrote the first draft. All authors contributed to the interpretation of the results, revised further drafts, and canonical the final manuscript.
Authors' original submitted files for images
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed nether the terms of the Artistic Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original piece of work is properly cited.
Reprints and Permissions
Virtually this article
Cite this article
Gurol-Urganci, I., Cromwell, D.A., Edozien, Fifty.C. et al. Gamble of placenta previa in second nascency afterwards first birth cesarean department: a population-based study and meta-analysis. BMC Pregnancy Childbirth xi, 95 (2011). https://doi.org/10.1186/1471-2393-11-95
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/x.1186/1471-2393-11-95
Keywords
- Cesarean Section
- Nativity Interval
- Placenta Previa
- Hospital Episode Statistics
- Previous Cesarean Section
Source: https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/1471-2393-11-95
0 Response to "If I Had Placenta Previa Will I Get It Again"
Post a Comment